Dental surgery - Questions & Answers
Piezosurgery is a modern surgical method that uses piezoelectric devices (i.e. ultrasonic cutters). These tools can successfully replace previously used bone cutters, chisels and other conventional instruments. Procedures performed with piezosurgery allow selective incision of bone tissues, minimizing the violation of soft tissues, which maximally reduces blood leakage during the procedure. After piezosurgical procedures, wounds heal faster and swelling is reduced. At our clinic, we work with the piezosurgical method using a state-of-the-art EMS piezoelectric scaler.
Tooth extraction during pregnancy is possible if necessary. The best time for this is the second trimester of pregnancy.
The decision on the number of teeth to be removed is made by the dentist after interviewing the patient. In general, there are no contraindications to removing more than one tooth at a time, as long as the patient does not have abnormalities on the side of the circulatory system (such as blood clotting problems) or other serious medical conditions.
Immediately after tooth extraction, one should refrain from drinking and eating for about two hours, so as not to flush out the clots forming in the alveolus after the extracted tooth. You should also refrain from smoking for the first 24 hours and from brushing your teeth for min. 8 hours. It is best to eat cold foods with a liquid consistency (such as yogurt) and drink large amounts of fluids (but avoid drinking through a straw). In addition, any physical exertion should be kept to a minimum. If necessary, you can take painkillers prescribed by your dentist and apply cold compresses to reduce swelling.
The decision to administer an antibiotic depends on the patient's overall health and the extent of the procedure. If the patient is healthy and the procedure was short, not extensive and went without complications, an antibiotic is not needed.
What to do if bleeding worsens after a tooth extraction?
Removal of the clot usually occurs due to too early intake of fluids after the procedure or rinsing the mouth with water. The empty space, unfilled by the clot, becomes a place for food debris and a habitat for bacteria. A local inflammation called “dry socket” develops. The post-extraction site then becomes very painful and heals very slowly. A dry alveolus requires wound care by flushing with an antiseptic and applying an analgesic/anti-inflammatory to the alveolus.
During the dental examination and consultation, the dentist will order the appropriate radiograph, which can be taken at the clinic on site. In the area of retained teeth, a pantomogram or CT scan will be reasonable (link to radiology).
In general, a typical tooth extraction does not require the patient to refrain from professional activity, unless it involves unusually heavy physical exertion. In special cases, such as extractions of retained teeth or removal of several teeth at a time, there may be indications to write the patient a medical exemption. The exemption is not mandatory, so it is always up to the dental surgeon performing the procedure to assess the indications.
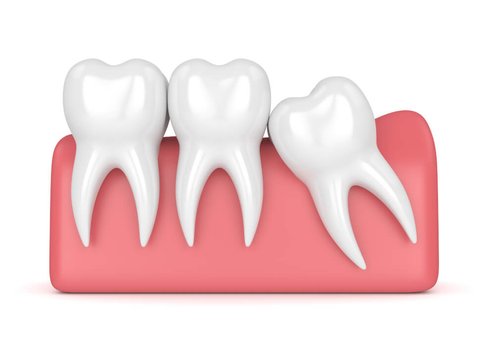
Not everyone has so-called wisdom teeth, and many people may have an incomplete set of them. The absence of visible eighths in the mouth does not mean they are not there at all, as they can be retained in the bone and not give any negative symptoms. If the eighth teeth are not visible to the naked eye, a panoramic photo of the jaw, or pantomogram (link to radiology), should be taken. The photo will show all teeth, including those retained in the bone.
When wisdom teeth do not give alarming signals (e.g., pain, inflammation, etc.) and there are no large carious cavities, there is no reason for extraction. Extraction should be considered in the case of teeth retained in the bone or abnormally positioned, as well as before orthodontic treatment when there is a lack of space in the dental arch with significant crowding of teeth in the anterior segment. Each time a recommendation for extraction of an eighth is preceded by a history, a thorough examination and photo documentation.
Theoretically, the extraction of eighth teeth can be performed by any dentist, nevertheless, in the case of these teeth, quite often we have to deal with unusual anatomical conditions (such as incomplete eruption) and it is reasonable that a specialist dental surgeon performs the procedure.
Sutures are placed when the surgeon, in order to extract a tooth, has to incise and dehisce the mucoperiosteal flap. Then the dissected tissues need to be sutured. If a fully erupted tooth is removed, without incising the flap, there is also usually no need for sutures. In our clinic, both traditional and dissolvable sutures are placed, depending on the clinical situation and the patient's ability to appear for suture removal.
As a rule, extraction of eights is performed under local anesthesia, but in special cases (e.g., severe dentophobia, strong vomiting reflex preventing any procedures, intellectual disability, some general diseases preventing the procedure under normal conditions), the procedure can be performed under anesthesia. The desire to perform the procedure under anesthesia should be announced in advance at the time of the consultation, as this requires an appointment with an anesthesiologist and is an extra fee service.
Theoretically, the removal of four eighth teeth during a single procedure is possible, but in practice it is rarely recommended and performed due to high postoperative discomfort for the patient. Most often in such a situation it is recommended to remove the eights by sides, that is, first the lower and upper eights on one side, and after a few weeks on the other side. This solution allows the patient to take meals while the post-extraction wounds heal.
In exceptional cases, four wisdom teeth can be removed at once, but then such a procedure is most often performed under general anesthesia (anesthesia) and is associated with significant postoperative discomfort for the patient.
The frenulum of the tongue is recommended to be undercut as soon as possible, in the first days of a baby's life. A frenulum that is too short can have an impact on the difficulty of breastfeeding the baby and the development of an abnormal sucking reflex. At later stages of development, a too-short frenulum can impede normal speech development, cause malocclusion or salivation. The procedure is usually performed by a pediatrician while still in the hospital, right after birth. However, if this defect is not detected then one should go to a periodontist or dental surgeon as soon as it is identified.
The frenulum of the upper lip, on the other hand, is usually operated on around the age of 8, after the four permanent incisors have grown. An upper lip frenulum that is too short or improperly attached can cause diastema (that is, a gap between the upper ones, caused by the separation of the teeth), lead to speech defects, and make it difficult to clean the teeth. Another serious complication can be inflammation of the gums and pulling of the gums, which can even lead to recession, or exposure of the root.